Medicine
Mar 23, 2026
Human Anatomy
Human Physiology
Biochemistry
Pathology
Pharmacology
Clinical Skills
Can a Gum Disease Bacterium Help Breast Cancer Spread? What the New Study Actually Shows
A new Johns Hopkins study suggests Fusobacterium nucleatum, a bacterium linked to gum disease, can reach breast tissue, accelerate tumor growth in mice, and worsen cancer-like beha
A bacterium best known for gum disease is now being discussed in breast cancer research, and the headline sounds almost unbelievable. But the deeper story is not that brushing your teeth prevents cancer. It is that microbes may sometimes act like hidden accelerants inside already vulnerable tissue. The new Johns Hopkins study is important because it proposes a mechanism, not just a correlation—and that mechanism raises serious questions for future human research.
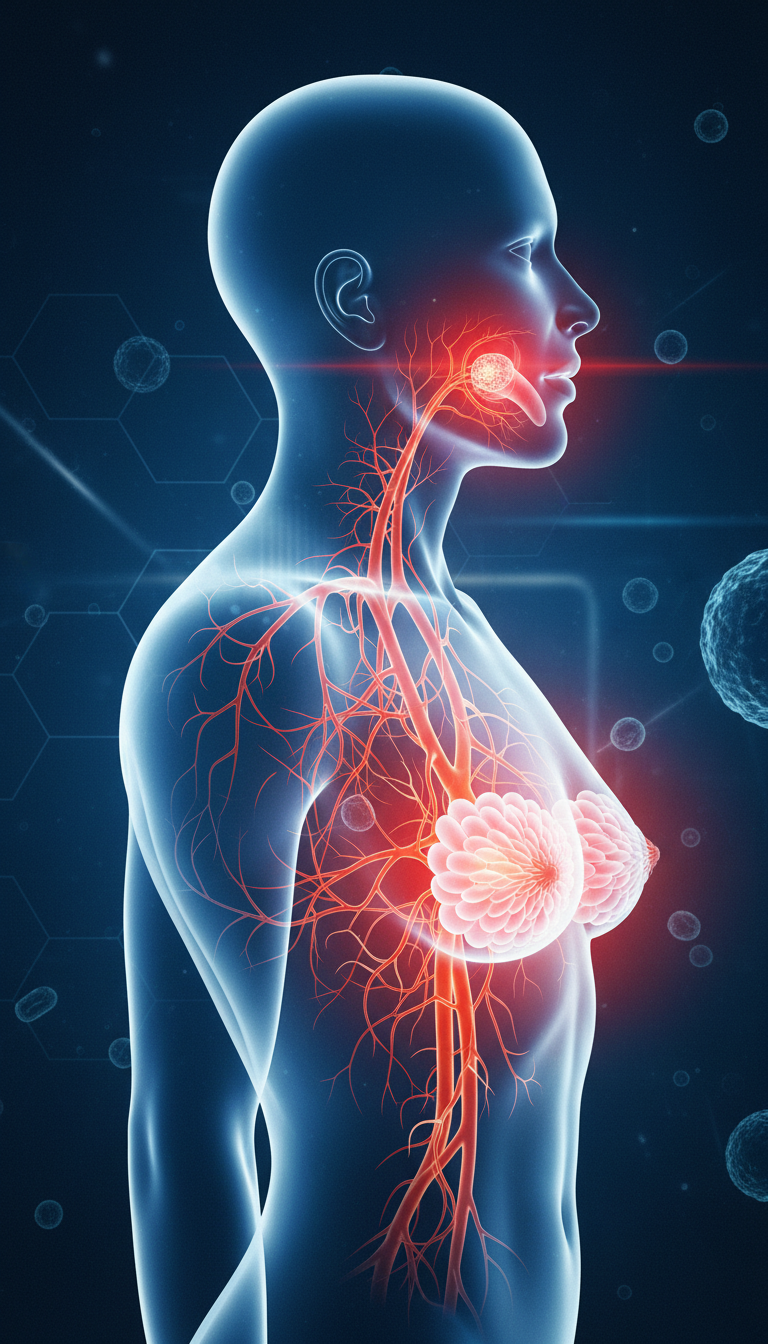
What the study found
The bacterium is Fusobacterium nucleatum, which has already been linked to colorectal cancer. In this new preclinical work, researchers reported that it could travel from the mouth through the bloodstream to breast tissue, where it promoted inflammation, DNA damage, abnormal cell growth, and faster tumor progression in mouse models.
The most striking results came in tumor-bearing mice: exposed tumors grew roughly three times larger over six weeks, and lung metastases appeared in all exposed mice in the experimental setting. In breast cancer cells, the bacterium also increased proliferation, migration, invasion, stem-like behavior, and resistance to chemotherapy.
That does not mean gum disease directly causes breast cancer in humans. It means this microbe may help existing cancer or precancerous tissue behave more aggressively under certain conditions.
How could a mouth bacterium affect the breast?
The proposed route is the bloodstream. Inflamed gums can allow oral bacteria to enter circulation more easily, especially during chronic periodontal disease. Once in the blood, F. nucleatum appears able to adhere to and enter certain breast cells.
Explore our free medicine courses
Human Anatomy
University · Medicine
Human Physiology
University · Medicine
Biochemistry
University · Medicine
Pathology
University · Medicine
Pharmacology
University · Medicine
Clinical Skills
University · Medicine
One reason this matters is persistence. The study suggests the bacterium can colonize breast cancer cells and remain inside them across cell generations. That is a much more consequential idea than a brief exposure. If confirmed in humans, it would mean the bacterium is not just passing through tissue but potentially reshaping tumor behavior from within.
Researchers also found that BRCA1-mutant cells were especially susceptible. These cells showed elevated Gal-GalNAc sugars on their surfaces, which may make bacterial internalization easier. In plain English: some genetically vulnerable cells may present a better “docking surface” for the bacterium.
Why BRCA1-mutant cells may be hit harder
BRCA1 is crucial for accurate DNA repair. When BRCA1 function is impaired, cells already have more trouble fixing genetic damage cleanly. The study suggests F. nucleatum makes that problem worse by pushing cells toward more error-prone repair pathways, including non-homologous end joining, associated with PRKDC activity.
That matters because error-prone repair can preserve cell survival while introducing new mutations. This may help explain why the bacterium was linked not only to faster growth, but also to invasion, stemness, and chemoresistance. In other words, the microbe may be nudging vulnerable cells toward a more chaotic and dangerous evolutionary path.
What evidence exists in humans so far?
The human evidence is still limited, but not empty. The researchers reported metagenomic evidence that F. nucleatum is overabundant in human breast cancer tissue. That supports the idea that the bacterium is present in at least some tumors, not just in mice or petri dishes.
Still, presence is not proof of cause. The key unanswered human questions include:
- Whether breast tumors containing more F. nucleatum have worse outcomes
- Whether patients with gum disease are more likely to harbor it in breast tissue
- Whether reducing periodontal disease changes cancer risk, progression, or treatment response
- Whether BRCA1 carriers are disproportionately affected in real-world populations
Those answers require clinical studies, not just lab models.
What this does and does not mean for patients
The practical takeaway is important but modest. This study does not justify replacing standard breast cancer prevention, screening, or treatment with dental interventions. It does not prove that antibiotics, flossing, or gum treatment will prevent breast cancer or stop metastasis.
What it does suggest is that oral health may be one more biologically meaningful piece of whole-body risk—especially in people with existing susceptibility. That makes dental care look less cosmetic and more medically relevant.
For now, the sensible response is straightforward:
- Keep up proven breast cancer screening and treatment.
- Do not ignore bleeding gums or chronic periodontal disease.
- If you carry a BRCA1 mutation, continue standard surveillance and genetic counseling; this research does not change those recommendations yet.
- Watch for future studies testing whether periodontal treatment or microbial targeting improves outcomes.
The bottom line
So how could a gum bacterium make breast cancer more dangerous? The new study suggests it can enter the bloodstream, colonize susceptible breast cells, and push them toward inflammation, DNA damage, and error-prone repair. And what happens next in humans? We do not know yet—but the most important next step is clinical research asking whether bacterial colonization tracks with outcomes and whether treating gum disease can change the course of risk or therapy response.






